-

-
About Us
- Our Vision
-
Personalized Care
Personalized Care Personalized Care Intro
Diagnostic Tests
- Digital X-Ray
- DynaROM
- 3D Body Scanning
- Gastrointentinal Health
- Organic Acids
- Comprehensive Stool Analysis
- Food Sensitivity
- Dietary Antigen Complete
- Endocrinology
- Thyroid Panel
- DUTCH Hormone Test
- Neurotransmitter Profile
- Adrenal Profile
- Nutritional Status
- Vitamin D
- Homocysteine
- Methylmalonic Acid
- Urine Iodine
- Organic Acids
- Copper Zinc Profile
- Essential Fatty Acid Profile
- RBC Metals & Minerals
- Toxic & Essential Elements
- RBC Elements
- Urine Toxic Metals
- Hair Metals & Minerals
- Urine Halides
Treatments
- Avacen Therapy
- Bioidentical Hormone Replacement Therapy (Anti-Aging)
- Chiropractic Care
- Electric Muscle & Nerve Stimulation
- Emsculpt Neo
- Emsella Treatment
- Erchonia Laser (Model EVRL)
- Exosomes
- Hair Restoration
- Headache & Migraine Treatment
- Hyaluronic Acid Injection
- Intersegmental Traction
- IV Nutrient Therapy
- Laser Lipo
- Massage Traction Chair
- PRP Facials
- PRP for Erectile Dysfunction
- PRP for Female Sexual Dysfunction
- PRP for Pain Relief
- PRP for Urinary Incontinence
- Semaglutide
- Shockwave Therapy for Cellulite & Skin Tightening
- Shockwave Therapy for Pain Relief
- Shockwave Therapy for Female Sexual Dysfunction
- Shockwave Therapy for Male Sexual Dysfunction
- Skin Rejuvenation
- Spinal Decompression
- TENS Unit
- Testosterone Replacement Therapy (TRT)
- Therapeutic Ultrasound
- Thyroid Care
- Trigger Point Therapy
- Durable Medical Equipment
- Ankle-foot Orthosis
- Cervical Rehab Coller
- Custom Foot Orthotics
- Lumbosacral Orthosis
- Osteoarthritis Knee Brace
- Wrist Brace
- FAQs
- Testimonials
- Pain Relief
- Weight Loss
-
Sexual Wellness
-
Anti-Aging
-
Resources
- Blog
- Video Library
- Store
-
Health Condition Library
Health Condition Library
- Ankle Osteoarthritis
- Bulging Spinal Disc
- Carpal Tunnel
- Cervical Degenerative Disc Disease
- Cervical Radiculopathy
- Elbow Bursitis
- Erectile Dysfunction
- Fatigue
- Female Hormone Imbalance
- Female Sexual Dysfunction
- Fibromyalgia
- Foot Arthritis
- Frozen Shoulder
- Golfer’s Elbow
- Hand Arthritis
- Headache
- Hip Bursitis
- Hip Osteoarthritis
- Hyperthyroidism
- Hypothyroidism
- Knee Bursitis
- Knee Osteoarthritis
- Low Testosterone
- Lumbar Degenerative Disc Disease
- Migraines
- Musculoskeletal Pain
- Obesity
- Osteoarthritis
- Plantar Fasciitis
- Plantar Fibroma
- Rotator Cuff Injury
- Sciatica Pain
- Shoulder Bursitis
- Shoulder Osteoarthritis
- Tennis Elbow
- Thoracic Degenerative Disc Disease
- Urinary Incontinence
- Weight Gain
- Wrist Arthritis
- Wrist Bursitis
- Contact
Understanding Sciatic Pain
Alternate Names: Sciatic pain is also referred to as sciatic neuritis, sciatic neuralgia, or lumbar radiculopathy. These terms are used interchangeably to describe the same condition.
Introduction:
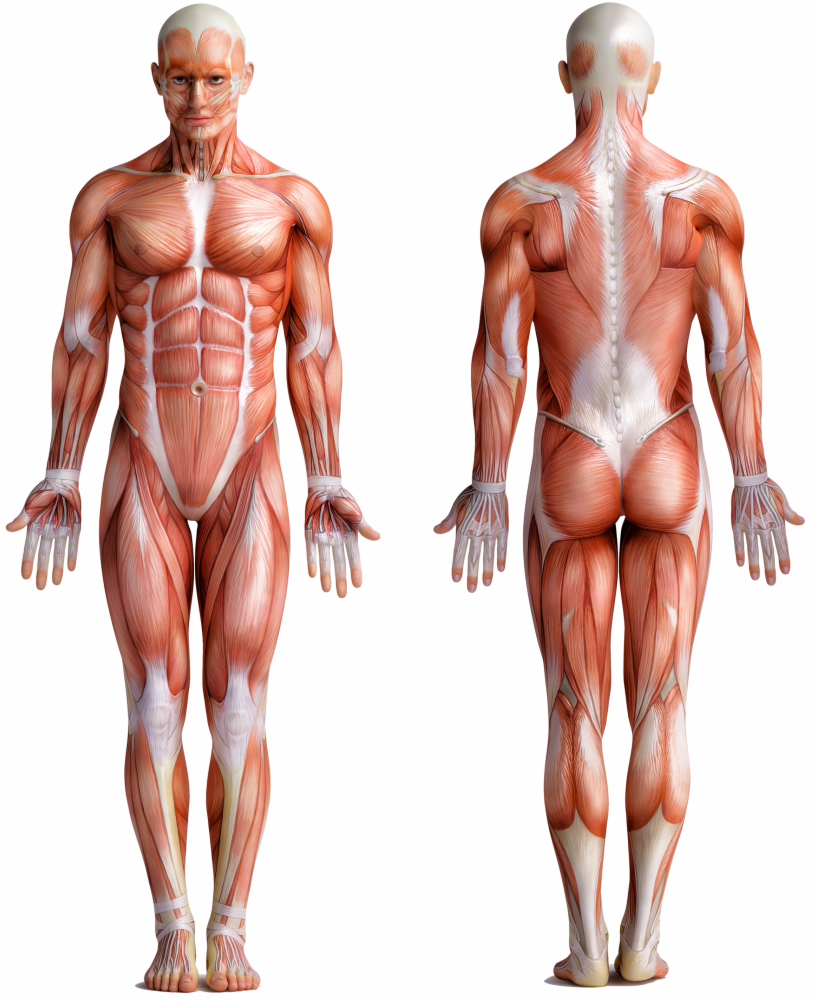
Sciatic pain is a common condition that affects many individuals worldwide. It is characterized by pain radiating along the sciatic nerve, which runs from the lower back, through the buttocks and into the legs. This comprehensive guide aims to provide expert insights into sciatica, including its alternate names, symptoms, causes and various treatment options.
Symptoms:
The hallmark symptom of sciatic pain is a sharp, shooting pain that travels along the path of the sciatic nerve. This pain can be felt in the lower back, buttocks, and down the back of the leg. Other common symptoms include numbness, tingling, or weakness in the affected leg or foot. Sciatica may become more painful with certain movements, such as sitting, standing or walking for prolonged periods.
Causes:
Sciatic pain is triggered by any condition causing compression or irritation of the sciatic nerve. This can occur due to various factors, including herniated discs, spinal stenosis, degenerative disc disease, or muscle imbalances. In some cases, underlying conditions such as diabetes or obesity may contribute to the development of sciatica.
Treatment Options:
There are several treatment options available for managing sciatic pain, depending on the severity and underlying cause. These include:
- Conservative Measures:
– Rest and activity modification.
– Physical therapy and exercises to improve flexibility and strengthen the core muscles.
– Heat therapy or cold therapy to ease pain and reduce inflammation.
– Over-the-counter medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs) to alleviate pain associated with the condition. Although Non-steroidal anti-inflammatory drugs (NSAIDs) do reduce inflammation to temporarily relieve pain, they are responsible for 30% of hospital admissions for adverse drug side effects, mainly due to bleeding, heart attack, stroke, and kidney damage. In addition, from the first day of use, all NSAIDs increase the risk of gastrointestinal (GI) bleeding, myocardial infarction, and stroke. - Medications:
– Prescription medications, including muscle relaxants or oral steroids, may be prescribed for more severe cases.
– In some instances, nerve pain medications or antidepressants may be recommended to manage chronic pain. - Injections:
– Epidural corticosteroid injections can provide temporary relief by reducing inflammation around the affected nerve. Side effects of cortisone, which is commonly injected for joint pain, includes thinning of the skin, easy bruising, weight gain, puffiness of the face, elevation of blood pressure, cataract formation, thinning of the bones, and a rare but serious form of damage to large joints (avascular necrosis). Due to risks, patients may only get this treatment once every several months.
– Nerve root blocks or facet joint injections may be considered for targeted pain relief. - Surgical Intervention:
– Surgery is typically reserved for cases where conservative treatments have failed to provide relief or if there is a significant underlying structural issue, such as a herniated disc.
– Surgical options may include discectomy, laminectomy, or spinal fusion, depending on the specific condition.
Conclusion:
Understanding sciatic pain is crucial for individuals experiencing its debilitating effects. By recognizing the alternate names, symptoms, causes, and treatment options, individuals can make informed decisions about managing their condition and seeking appropriate medical care. It is advisable to consult with a healthcare professional for a precise diagnosis and personalized treatment plan.